Clinical Immunology and Allergy is a specialty within Internal Medicine recognised by the Australasian College of Physicians. Specialists diagnose and treat immune system conditions, including:
- Allergic disorders: food allergies, hay fever, hives (urticaria), anaphylaxis, venom allergy, atopic eczema, and allergy-related asthma
-
Autoimmune disorders: systemic lupus erythematosus (SLE), Sjogren’s syndrome, scleroderma, myositis, and vasculitis
-
Immunodeficiency disorders
-
Chronic fatigue syndrome
-
Periodic fever syndromes
Allergy Testing
The Allergy Clinic at Specialist Medical Randwick offers comprehensive skin prick tests for aeroallergens every Monday 8:30 AM – 5:00 PM.
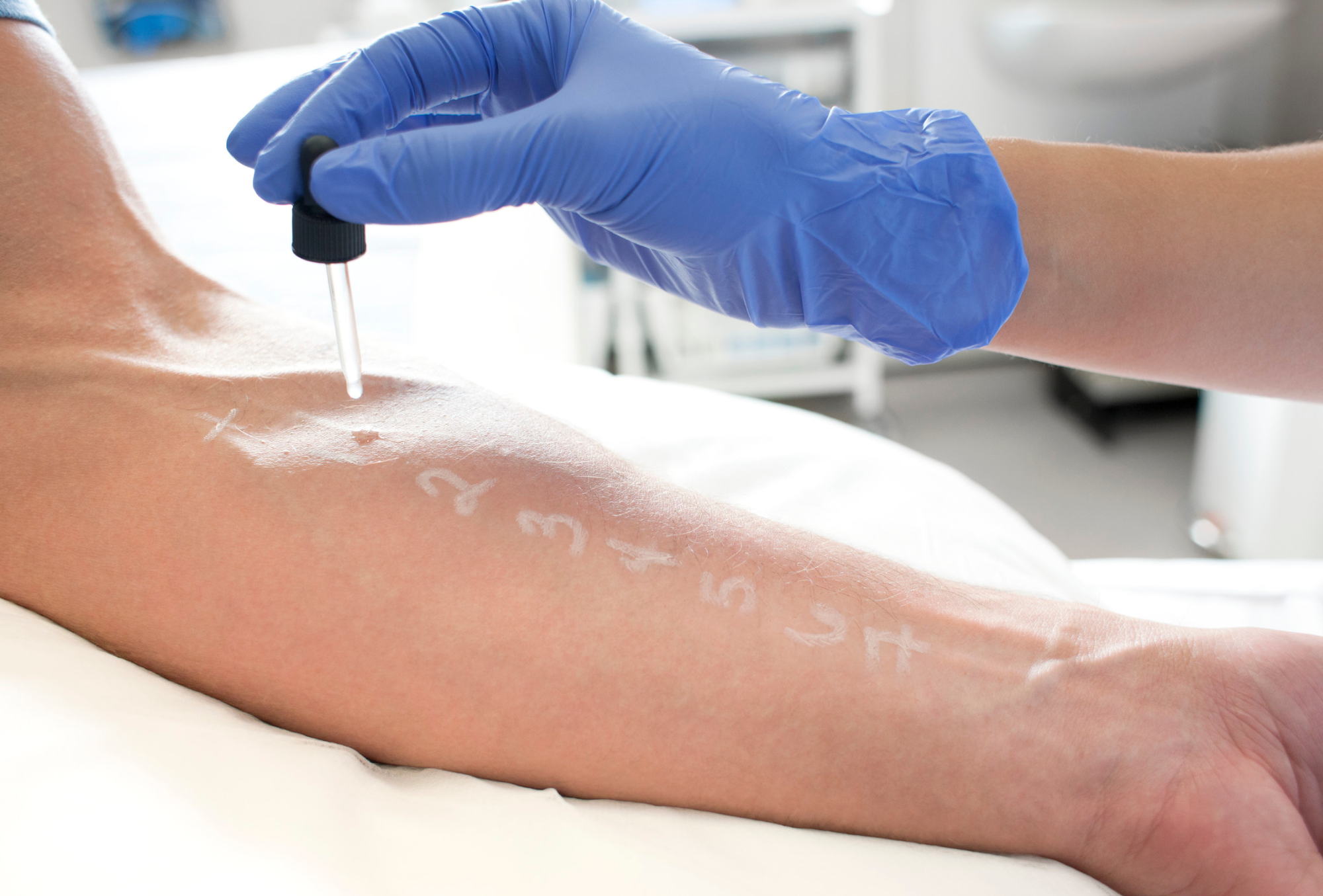
Skin prick testing for allergies
Skin prick testing is a quick, accurate, and affordable way to identify allergies, with results available within 20 minutes.
During the test, a small drop of allergen extract is placed on your forearm (or back in young children), and a sterile lancet gently pricks the skin. If you’re allergic, a small itchy bump (wheal) will appear, which usually settles within 1–2 hours.
Severe reactions are very rare. To ensure accurate results, avoid antihistamines and related medications for 3–7 days before your appointment, and don’t apply creams or moisturisers to your forearms on the day of testing.
If skin testing isn’t suitable (for example, due to severe eczema or interfering medications), a blood test for Immunoglobulin E (IgE) antibodies can be performed instead.
Patch testing
Patch testing helps identify contact allergic dermatitis, such as reactions to metals or cosmetic preservatives.
A small amount of allergen paste is applied to the skin (usually on the back) using hypoallergenic tape. The patches remain in place for 48 hours and must be kept dry.
After removal, any eczema-like rash indicates sensitivity to a specific allergen.
Challenge testing
Challenge testing is used to confirm or rule out allergies when the cause of a reaction is uncertain or to check if an allergy has resolved.
This test is performed under strict medical supervision, using controlled exposure to foods or medications in a safe environment with resuscitation facilities available.
Autoimmune Testing
Autoimmune diseases occur when the immune system attacks the body’s own cells, leading to inflammation and tissue damage.
They may affect one organ (such as the thyroid) or multiple systems (such as lupus or vasculitis).
Autoimmune diseases are usually diagnosed and monitored using the clinical history, blood tests (autoantibodies, inflammation, organ function) and other investigations such as radio-logic and nuclear medicine imaging.
While there is currently no cure, various treatments — including non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroids like Prednisolone, and other immunosuppressive medications — can help manage symptoms and reduce disease activity, depending on the type and severity of the condition.
Immunodeficiency Testing
People with immunodeficiency are more prone to recurrent, persistent, or unusually severe infections, which can sometimes lead to organ damage.
Diagnosis is typically made through blood tests that assess antibody (immunoglobulin) levels, lymphocyte count and function, complement levels, and phagocyte activity. Treatment options may include immunoglobulin replacement therapy, immune modulation, and antimicrobial medications.